Why Cultural Competence is Important in Healthcare
Cultural competence is growing a focus in all industries including healthcare. The American Hospital Association (AHA) defines a culturally competent healthcare system as one that “acknowledges the importance of culture, incorporates the assessment of cross-cultural relations, recognizes the potential impact of cultural differences, expands cultural knowledge, and adapts services to meet culturally unique needs.” Cultural competence is so important in healthcare settings because it aims to reduce racial, economic, ethnic, and social disparities when meeting a community’s health care needs.
How can I develop cultural competence as a nurse?
Developing a culturally competent healthcare environment starts with awareness of your own cultural background and experiences. No matter what your upbringing looked like, we all carry certain biases based on our cultural backgrounds. As a nurse, it is important to limit the influence of these biases when interacting with patients whose identities and life experiences differ from your own.
Beyond this starting point, cultural competence requires an understanding of and respect for other cultures. It is important to educate yourself and be open to learning patient’s backgrounds to effectively meet their care needs. For example, learning about a Muslim patient’s prayer schedule and planning infusions around their prayer times will allow them to feel seen and supported during their hospital stay.

Focusing on Patients’ Cultural Needs
The American Nurses Association (ANA) Code of Ethics states that nurses must “practice with compassion and respect for the inherent dignity, worth, and unique attributes of every person.” The only way to treat all patients with compassion and dignity is by understanding their cultures and responding appropriately to their needs. Unfortunately, this often does not happen in practice. The following three examples from a Regis College blog post demonstrate how a lack of cultural understanding may add to a patient’s stress:
● A Native American man tells emergency room staff he is following the “old ways” of dying and asks that his family be around him. Instead, he is transferred to an intensive care unit (ICU) hundreds of miles away for the extensive treatment he did not want, and his family cannot join him. He dies two weeks later, after being resuscitated twice, and his wife is the only family member with him.
● A Chinese patient admitted to the ICU after heart surgery asks the medical staff to allow his wife to cook a therapeutic meal for him that contains special herbs and that only his wife knew how to make. His nurses did not understand his initial request, after which he stopped asking because he was afraid of how they might view him.
● A newborn is too ill to be discharged with his Vietnamese mother, and the nursing staff becomes concerned that the mother appears not to be bonding with her new baby. A specialist in transcultural nursing care explains to the staff that in rural Vietnam, many people believe spirits are attracted to and may harm newborns, so they try not to draw attention to babies. What had seemed to the staff as uncaring was in fact a reflection of the mother’s love for her child.
Important Skills for Cultural Competence
Nurses with strong leadership and communication skills are needed to successfully implement cultural competence in healthcare settings and avoid these situations. Addressing the needs of underserved communities requires that nurses recognize and adapt to the social, ethnic, and linguistic needs of the people in these communities. This includes:
● Participating in lifelong learning to understand the cultural preferences, worldview, choices, and decision-making processes of patients.
● Communicating with appropriate language and behaviors, including the use of medical interpreters and translators.
● Educating fellow nurses and colleagues about cultural similarities and differences patients, families, groups, communities, and populations.
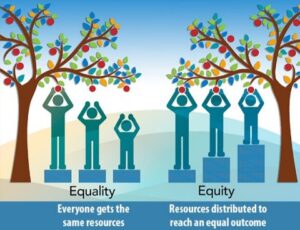
Cultural Competence Beyond Healthcare Settings
RNs are on the front lines of integrating cultural competence not only in healthcare settings, but also in their communities. Nurses have the opportunity to promote cultural competence principles in their communities through initiatives to improve healthcare access and equity (defined below) for vulnerable groups. Informed by their work in hospitals and clinics, many RNs are invested in the uplift of marginalized groups. Culturally competent nurses are the key to making change at the ground floor, which is why they are becoming increasingly important in the healthcare world and beyond.