Understanding and Navigating the Nurse Shortage
Why is there a nurse shortage?
It’s no secret that the healthcare world is experiencing a shortage of one of its main resources: nurses. While it’s tempting to think of COVID-19 as the key driver of the nurse shortage, that’s not the whole reason. The high stress of working during a pandemic has certainly exacerbated the problem, but the nurse shortage was already a concern well before COVID-19 hit the United States and will likely continue to be a concern for years to come. There are a number of factors driving this shortage, including a retirement boom, lack of educators, and of course, burnout.
WorldWide HealthStaff Solutions
The retirement boom
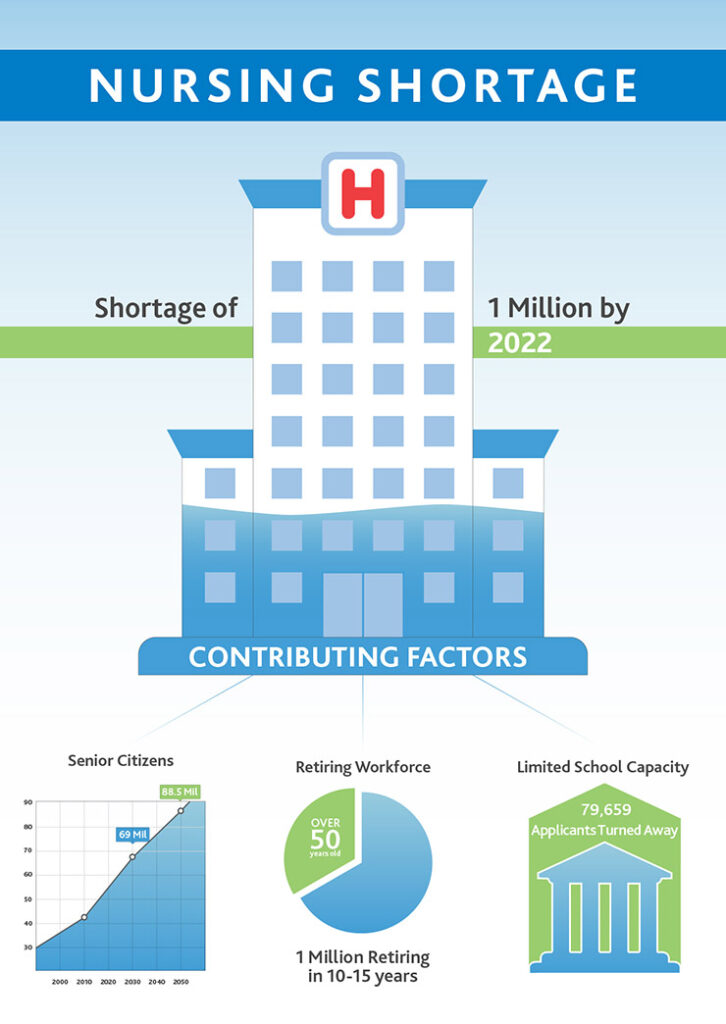
The retirement boom among older nurses has created thousands of job openings in nursing. The massive increase in job openings has coincided with an increase in the number of patients seeking healthcare, and there simply aren’t enough new nurses entering the workforce each year to keep pace with these rising rates.
The Bureau of Labor Statistics expects the RN workforce to grow by an average of 30,000 new nurses per year from 2019–2029, which is nowhere near enough to meet the Bureau’s projection of 175,900 openings each year over the same time period. Studies have projected that 1.2 million more nurses will be needed by 2030 in order to keep pace with this high demand, creating a nurse shortage.
Shortage of nursing educators
The nurse shortage is a big enough problem on its own, but there is an underlying factor that has exacerbated the issue: a shortage of educators. Nursing schools across the country are experiencing a faculty shortage, which limits the number of nursing students schools can accept.
A report from the American Association of Colleges of Nursing found that in 2019, U.S. nursing schools turned down 80,407 qualified applicants for nursing programs. The main reasons were insufficient numbers of faculty members, not enough clinical sites or classroom space, and budget constraints. A separate survey found that nursing schools not only needed to create more faculty positions to accommodate demand, but that they were struggling to fill existing faculty vacancies.
Job stress and clinician burnout
Nursing is a high-stress profession under the best of circumstances, and burnout is definitely a driving force behind the nurse shortage. Nurses not only have to deal with an increasing workload, but they have to do it while also dealing with human suffering and loss of life on a regular basis. On top of that, because nurses interact directly with patients more than any other provider, they are at the highest risk of workplace violence of any healthcare professional, causing many nurses to discontinue practicing. Nurses universally agree that theirs is an incredibly rewarding profession but can be an unforgiving one.

The impact of the nurse shortage
Patients and their families are definitely feeling the impact of the nurse shortage, as it affects the quality of care they receive. At the heart of it, a nurse shortage means there are fewer nurses caring for an increasing number of patients. Fewer nurses means a higher risk of adverse events that are commonly associated with overworked and under-supported nursing staff within a healthcare organization including: medication errors, negligence, even patient death.
Solutions for the nurse shortage
Having a better understanding of the problem is an important first step toward solving it, but what can actually be done to reduce the nurse shortage in healthcare organizations? Here are a few key solutions that could help bring this problem under control.
Strategic workplace accommodations
It’s an inescapable fact that nurses are overworked. 83% of nurses cited poor work/life balance as the main reason that hospitals and healthcare organizations are losing good nurses. Healthcare organizations and leaders may not be able to do much to reduce nurse workloads, but there are things they can do to help make life a little easier for overworked nurses in the meantime.
Healthcare leaders should consider implementing strategic workplace accommodations to help nurses more effectively manage job stress. These accommodations can vary depending on the specific needs of an organization’s nursing staff, but examples include allowing nurses additional break time during their shifts to de-stress or holding group sessions to talk about mental health . Healthcare organizations can also create physical space where nurses can go to take a breather when things get hectic.

Workforce solutions & flexibility
Additional flexibility also goes a long way toward restoring work/life balance for an organization’s nursing staff. The easiest way for leaders to provide that flexibility is to actually listen when nurses voice concerns about high patient loads or feeling overwhelmed and do everything they can to reduce those stressors. Effective staffing, technology, and workforce management can be a great way to build in this flexibility without increasing the workload for other nurses. It is imperative that we make our clinical settings less stressful in order to remediate the nurse shortage.